DNA errors and new mutations in the melanin-producing cells – melanocytes – give rise to a tumor called melanoma. The most frequent cause for this malignancy is excessive exposure to ultraviolet radiation while sunbathing or indoor tanning.
The other risk factors include heredity, light skin type, high amount of moles on the body (over 50) and immunosuppresion. The latter is mostly caused by HIV or by immunosuppressive medications.
In the last century the number of skin cancer is increasing. Maybe this is happening because the beauty standards are changing ?
Earlier in the days pale skin was associated with royalty and higher status. People that worked in the fields more often had tanned skin. On the other hand, the nobles didn‘t have to go outside and work for a living. For that reason they received less UV overexposure and had fair-skin. Interestingly, some places like the majority of Asia (particularly Thailand) still consider pale skin as a beauty ideal.
However, nowadays in the west a tanned body is being regarded as a symbol of youth, beauty and sexuality. It is no surprise that so many people spend hours in tanning beds. Perhaps it is not emphasized enough that such an innocent thing such as indoor tanning can double the likelihood of melanoma. Besides, did you know that the World health organization classified ‘‘Ultraviolet-emitting tanning devices“ as a first group cancerogen? (Ref.)
It is worth remembering that even such a simple thing like a sunscreen can literally be lifesaving. Some sources claim that UV protection could reduce the risk of skin cancer at least by 50 %.
To our surprise, melanoma accounts only for 5 % of all skin cancers. However, it is responsible for at least 75 % deaths related to the malignancies of the skin. No wonder why such a relatively rare cancer is so reknowned.
| Melanoma | |
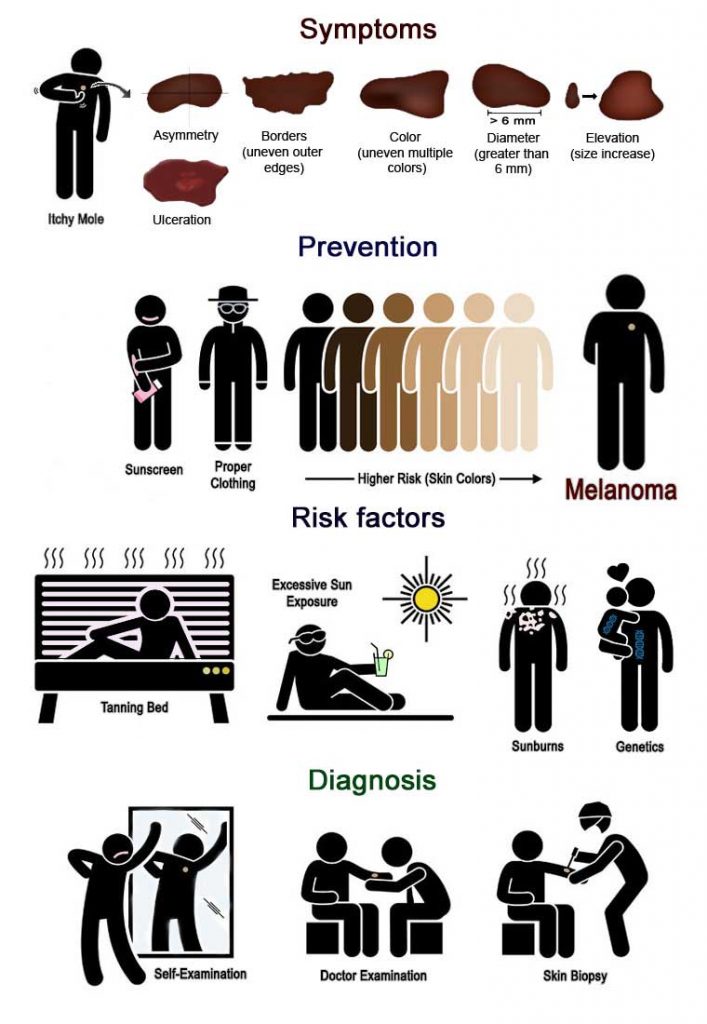
| Symptoms | Suspicious mole features (ABCDE rule): A – Asymmetry. One side of the mole differs significantly from the other side. B – Borders. The borders of a possible melanoma can be irregular, unclear, scalloped, notched and uneven. C – Color. A questionable mole can be unevenly colored and have different shades. There can be variations of white, grey, black, pink and blue. D – Diameter. A malignant melanoma can be small, however, in most cases it is wider than 6 mm (a size of a pencil eraser). E – Elevation (growth). If a mole changes its size, shape or texture in a couple of weeks or months, it should raise concern. (Ref.) • Ulceration can also develop, it can be a warning sign of melanoma. Redness, swelling and pigmentation are also signs that should raise a concern. • Bleeding and fluid excretion of a mole and its surroundings are also alarming signs. • The mole can become itchy and painful. Lesions and scabs can start forming. In this case get a skin check at a dermatologist or another specialized doctor. |
| Diagnosis | Regularly check your body surface and apply the ABCDE rule. Significant attention should be directed towards dysplastic nevi (1 out of 100 can become cancerous), common moles that change (1 out of 3 000 can become cancerous) and newly appeared growth on the skin. (Ref.) The ugly duckling sign. A suddenly appeared melanoma is very often different than the rest of the moles on the individual‘s body. (Ref.) Regular skin checks and follow-up appointments. If you have risk factors or had melanoma – booking at least one visit to the doctor‘s office a year could be a great investment. The best prevention is to have a suspicious mole checked and removed if needed. Questionable moles are examined with a dermatoscope and other tools. Melanoma is confirmed when a skin biopsy is done. If there are speculations that the cancer has spread, the sentinel lymph nodes are checked. CT, MRI or PET scans can also be performed to get a complete systemic image. |
| Prevalence | 87 000 new melanoma cases in USA every year. Melanoma accounts for 5 % of all new diagnosed cancers every year. |
| Age groups | The average age when melanoma appeared – 50 – 55 years. The lowest prevalence of melanoma is in the 20 – 34 year group (6% of all cases). The highest prevalence of melanoma is in the 55 – 74 year group (45% of all cases). (Ref.) |
| Treatment | Depends on the stage of the cancer. A melanoma that has not spread is removed surgically. A melanoma that has spread to the lymph nodes – the tumor is removed surgically following by the removal of sentinel lymph nodes and systemic treatment. Advanced melanoma (metastatic) is treated systemically with interferon, chemotherapy, medications that block signal molecule, angiogenesis inhibitors, immunotherapy. BRAF mutation is a valuable sign in choosing the best treatment. The majority of the systemic treatment options can cause side effects, the effectiveness greatly depends on the genetics of the individual. |
| Prognosis | The earlier melanoma is caught and removed surgically – the better the outcome. Early stages of melanoma have an almost 100 % cure guarantee. Advanced melanoma has a poorer outcome, it can be improved with the help of systemic treatment (including Sodium dichloroacetate). Prognosis calculator: http://www.melanomaprognosis.net/ |
If you belong to a risk group – you have a fair skin tone, more than 50 moles, someone in your family tree had melanoma, you take immunosuppressive drugs regularly or had serious sunburns in your life – please develop a habit to examine your skin regularly every month or so.

As with the majority of cancer cases, time is of the essence with melanoma.
The sooner it‘s noticed – the better the outcome. Moreover, melanoma can simply be noticed with the help of self-examination in front of the mirror. This makes it one of the most easily and early noticed tumors there is. In many instances, one can spot melanoma without the help of a doctor.
To treat advanced melanoma, one must use systemic whole body affecting medications. Currently the most popular choices in conventional medicine are chemotherapy, immunotherapy and target therapy. The latter two are new methods and grant hope in metastatic melanoma treatment. Then again, a lot of work still needs to be done in the pursuit of better therapy against this neoplastic disease. (Ref.) What we described are the main treatment options used by doctors in ordinary clinical settings. Naturally, there are other additional ways that may help stabilize or shrink the tumors.
With this in mind, let‘s look at the other options available widely for people with cancer .
Truly, while there are surgical, medical or dietary methods to fight melanoma, one shouldn‘t forget another considerable option – metabolic therapy with dichloroacetate. The tiny molecule which exhibits selective cytostatic and cytotoxic effect on cancer cells.
Alternative Treatment Approache for Melanoma – Sodium Dichloroacetate (DCA)
Today the publicly available evidence states that DCA could be useful against brain, thyroid, lymphoma, neuroblastoma, breast, lung, kidney, colon and other cancers. (Ref.)
To our surprise, Sodium dichloroacetate also seems to be effective in the treatment of advanced melanoma. It appears to have the capacity to shrink tumors, stabilize the disease and to prevent the condition from worsening. All of which happened in this example with a man from Canada.
We present a clinical case – BRAF-positive, III stage recurrent melanoma, which continuously came back after a handful of conventional medicine treatments.
Clinical Case: Sodium Dichloroacetate Therapy for Advanced Melanoma
In a period of 4 years dichloroacetate helped the man not only to stabilize the disease and shrink the existing cancerous masses, but also to continue living a normal life while experiencing minimal side effects. (Ref.)
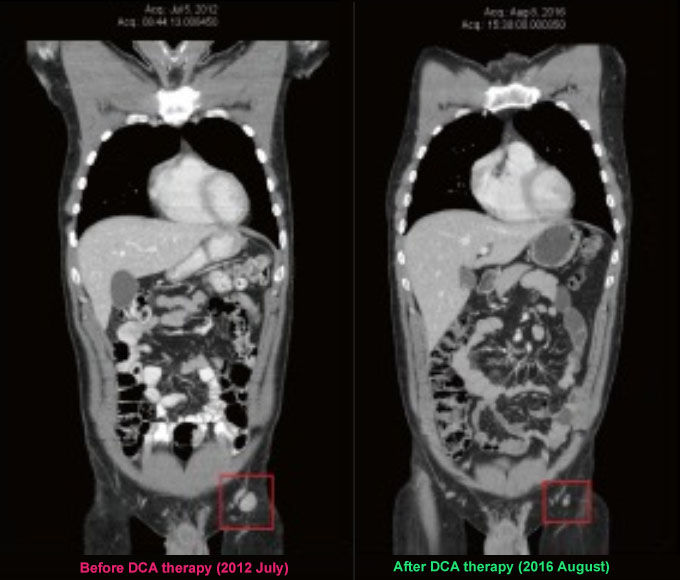
It all began in 2006 when this 32 year old fair-skinned man noticed a changing mole on his leg. The skin lesion looked like it should be checked out by a specialist. Little did he know that this small surprise would later become a big problem and regularly come back every time it was treated. Bigger, meaner and more stubborn.
The person visited the doctor and had a skin check. The dermatologist confirmed the lesion to be cancerous and soon afterwards it was removed by a surgeon‘s scalpel. The pathologists identified the excised skin tissue to be melanoma. Luckily, the disease hadn‘t spread to the nearby lymph nodes by then. There were no more suspicious moles.
After a year the male noticed enlarged lymph nodes in his groin and new melanoma-like looking lesions on his left leg. It looked like the cancer had relapsed. Shortly, after a visit to the hospital the man was prescribed Interferon-Alpha and began systemic treatment.
Thankfully, the results were not bad. The Interferon-α therapy lasted 9 months and it shrank the enlarged cancerous lymphoid tissue as well as the malignant melanoma on his leg. However, the treatment made the man feel sick, he couldn‘t bear the flu-like side effects. Therefore, he stopped taking the medication.
Till 2010 the man had no bigger complains regarding his health and lived on. Sadly, the cancer reappeared again. The male noticed new skin cancer lesions on his left leg, which were once again removed in a health care center surgically.
Despite the efforts, at the end of 2011, the melanoma lesions recurred in the same place again. This time they grew on the scar tissue formed from the last surgical operation. At this point the surgeons decided to remove a broader area of the skin with the recurrent tumors and to perform a skin grafting operation.
Unfortunately, at 2012 March the tumors reappeared in the new skin graft. The doctors tried to perform two more skin removal operations and skin grafting procedures, but it was no use. The cancer relapsed every time. A biopsy of the left groin lymph nodes was made.
The biopsy confirmed the metastasis of BRAF-positive melanoma to this region. The man fought 6 years against this deadly disease, had at least 5 surgical operations and even took systemic treatment. Sadly, every year the skin cancer would renew itself and everything started over again.
After a couple of months he started looking for alternative cancer treatment methods – he took a vegan diet and was consulted by a naturopath. The Naturopathic doctor prescribed:
• mushroom extract (with the active compound AHCC), • dandelion root, • astragalus root,
• curcumin, • European mistletoe extract, • intravenous vitamin C.

Regardless of the hopeful and enthusiastic attempt, the vegan diet and the naturopathic therapy didn’t seem to work. After a couple of months CT and PET scans revealed that the cancerous tumors are growing and the lymph nodes in the inguinal region are getting larger.
Not only the cancer was spreading, but also an aching pain appeared in the area of the enlarged lymph nodes.
Cancer screening tests revealed that the patient had disease progression.
With nothing to lose, the man decided to try out the DCA therapy, which recently had generated community interest in Canada.
2012 July, approximately 6 years after the cancer diagnosis and various treatment approaches, the male once again decided to overcome his stage III melanoma. This time with the help of Sodium dichloroacetate.
His every day ‘‘DCA protocol‘‘ consisted of:
• 500 mg of DCA three times a day
(administration scheme (cycles) – 2 weeks of DCA intake + 1 week break),
• 80 mg of Benfotiamine twice a day,
• 150 mg of Alpha-Lipoic acid three times a day,
• 500 mg of Acetyl L-Carnitine three times a day.
He took this mixture for four years. During this time period, he experienced mild side effects. The man felt slight numbness and weakness in his fingers and hands at some point, he also noticed gentle concentration disturbances.
However, it didn‘t take long till he reversed the adverse reactions. This was most likely achieved because of switching to a different administration scheme – 2 weeks on DCA + 1 week off DCA. Secondary responses weren‘t experienced later on.
Perhaps an additional week break is sufficient enough to give the body adequate time to flush away the accumulation of DCA. Furthermore, the 14 days of continuous Sodium dichloroacetate intake is more efficient in selectively getting rid of cancer cells (more about the administration schemes). The man also performed regular blood tests to make sure that everything is okay. Even when administrating dichloroacetate for four years, the parameters continued to stay within normal ranges. The slightly decreased creatinine levels were already noticed before the DCA protocol, moreover, this modest change is not clinically significant.
The example of blood work proves that when one takes Sodium dichloroacetate for long periods of time, noticeable toxic effects on the majority of organ systems don‘t seem to be evident.
I was able to find good information from your content.